Resources
Using Rate Review to Address Heathcare Affordability
Rate review is the process by which insurance regulators review health carriers' proposed insurance premiums to ensure they are based on accurate, verifiable data and realistic projections of healthcare costs and utilization.
States deploy a variety of approaches ranging from states that have received an “ineffective” designation from the federal government to states that expose the full filing, have robust public engagement and utilize a wide variety of factors in their review.
Consumers would be surprised to learn that regulators typically do NOT take affordability into account when reviewing rates. Instead, the typical factors taken into account might include: rates cannot be excessive, inadequate or unfairly discriminatory.
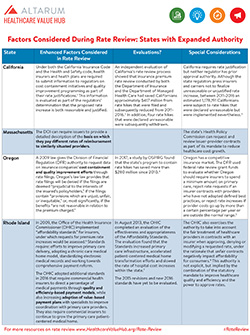
But as the table below shows, a few states go further (PDF version).
| State | Enhanced Factors Considered in Rate Review | Evaluation? | Special Considerations |
| California | Under both the California Insurance Code and the Health and Safety code, health insurers and health plans are required to submit information to regulators on cost containment initiatives and quality improvement programming as part of their rate justifications.1 This information is evaluated as part of the regulators’ determination that the proposed rate increase is both reasonable and justified. | An independent evaluation of California’s rate review process showed that insurance premium rate review conducted by both the Department of Insurance and the Department of Managed Health Care had saved Californians approximately $417 million from rate hikes that were filed and subsequently reduced from 2011-2016.2 In addition, four rate hikes that were declared unreasonable were subsequently withdrawn. |
California requires rate justification but neither regulator has prior approval authority. Although the state regulators press insurers and carriers not to finalize unreasonable or unjustified rate increase, between 2011-2016 an estimated 1,178,191 Californians were subject to rate hikes that were declared unreasonable but were implemented nevertheless.3 |
| Massachusetts | The DOI can require issuers to explain the extent of price variation between participating providers and describe any efforts to reduce such variation.4 | The state’s Health Policy Commission can request and review issuer-provider contracts as part of its mandate to reduce healthcare cost growth. | |
| Oregon | A 2009 gives the Division of Financial Regulation (DFR) authority to request data on insurance companies’ cost containment and quality improvement efforts through rate filings. Oregon law provides that rate filings will be denied if the filings are deemed “prejudicial to the interests of the insured’s policyholders,” if the filings contain “provisions which are unjust, unfair, or inequitable,” or, most significantly, if the benefits “are not reasonable in relation to the premium charged.” | In 2017, a study by OSPIRG found that the state’s program to contain rate hikes has saved more than $280 million since 2010.5 | Oregon has a competitive insurance market. The DFR used federal rate review grant funds to evaluate whether Oregon should require insurers to spend a minimum amount on primary care, reject rate requests if an insurer contracts with providers who have not adopted defined best practices, or reject rate increases if provider costs go up by more than a certain percentage per year or are outside the normal range.6 |
| Rhode Island | In 2009, the Office of the Health Insurance Commissioner (OHIC) released a set of “Affordability Standards” for insurers, under which their requests for premium rate increases would be assessed.7 Standards require: efforts to improve the delivery of primary care, adopting a chronic care model of medical home, standardizing electronic medical records and working towards comprehensive payment reform. The OHIC revised the Affordability Standards in 2015 and adopted additional standards in 2016. The new standards require commercial health insurers to direct a percentage of medical payments through quality and efficiency-based payment models, while also increasing adoption of value-based payment plans with specialists to improve coordination with primary care providers. They also require commercial insurers to continue to grow the primary care patient-centered medical home. | In August 2013, the OHIC completed an evaluation of the effectiveness and appropriateness of the Affordability Standards. The evaluation found that the Standards increased primary care infrastructure, accelerated patient-centered medical home transformation efforts and slowed the rate of hospital cost increases within the state.8 The 2015 revisions and new 2016 standards have yet to be evaluated. | The OHIC also exercises the authority to take into account the fair treatment of healthcare providers in contracts with an insurer when approving, denying or modifying a requested rate, under the rationale that unfair contracts negatively impact affordability for consumers.9 This authority is not explicit, but implied by the combination of the statutory mandate to improve healthcare quality and efficiency and the power to approve rates. |
| Vermont | The Green Mountain Care Board (GMCB)10 considers affordability when reviewing proposed health insurance rates, in addition to whether the rate “promotes quality care; promotes access to health care; protects insurer solvency; is not unjust, unfair, inequitable, misleading or contrary to law; and is not excessive, inadequate or unfairly discriminatory.”11 | An independent evaluation of Vermont’s rate review process revealed that total premium rate adjustments saved Vermonters approximately $66 million from 2012-2016. Additionally, average carrier administrative costs as a percentage of premium decreased significantly and became more consistent. | |
| Washington |
The Office of the Insurance Commissioner has authority to review insurer-provider contracts, as well as downstream entity contracts. In 2008, the Office of the Insurance Commissioner regained the authority to review health insurance rates. It disapproves any form or rates if the benefits are unreasonable in relation to the premium charged. It also adopted rules in 2014 and 2016 that increased its authority over insurers’ provider contracts and their networks. |
||
|
1. Insurance Code 10181.3(c)(3) and Health and Safety Code Section 1385.03(c)(3). |
|||
More resources
- CMS: Review of Insurance Rates
- STUDY: States with Stronger Health Insurance Rate Review Authority Experienced Lower Premiums in the Individual Market in 2010-2013, Health Affairs (August 2015)
- STUDY: The Association of State Rate Review Authority with Health Insurance Premiums, HCFO (2015)
- STUDY: Rate Review: Spotlight on State Efforts to Make Health Insurance More Affordable, Kaiser Family Foundation (2010).