Tennessee Residents Struggle to Afford High Healthcare Costs, Particularly in Rural Areas
A survey of more than 900 Tennessee adults, conducted from March 26, 2021, to April 9, 2021, found that people living in rural Tennessee experience greater healthcare affordability burdens than people living in non-rural areas of the state. Almost 7 in 10 (67%) of rural adults experienced one or more of the following healthcare affordability burdens in the prior 12 months, compared to almost 6 in 10 non-rural residents:
1) Being Uninsured Due to High Premium Costs1
2) Delaying or Forgoing Healthcare Due to Cost
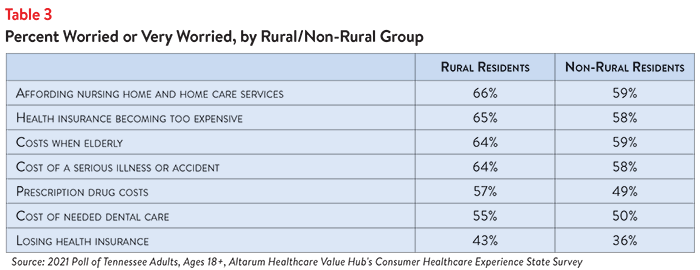
Six in ten rural Tennessee adults (60%) encountered one or more of the following cost-related barriers to getting healthcare during the prior 12 months, compared to 49% of non-rural Tennessee adults.
Moreover, cost was by far the most frequently cited reason for not getting needed medical care for both non-rural and rural residents, exceeding a host of other barriers like transportation, difficulty getting an appointment and lack of childcare.
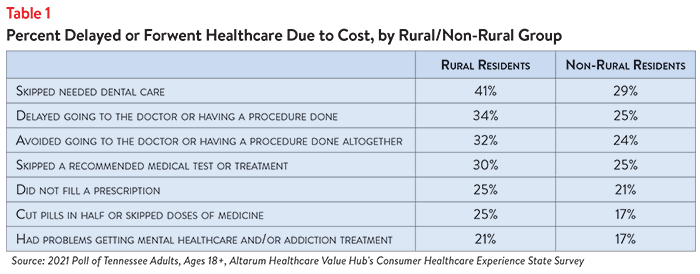
3) Struggling to Pay Medical Bills
Other times, Tennessee adults got the care they needed but struggled to pay the resulting bill. Almost half (42%) of rural Tennessee adults experienced one or more of the following struggles to pay their medical bills in the prior 12 months, compared to 31% of non-rural Tennessee adults:
High Levels of Worry About Affording Healthcare in the Future
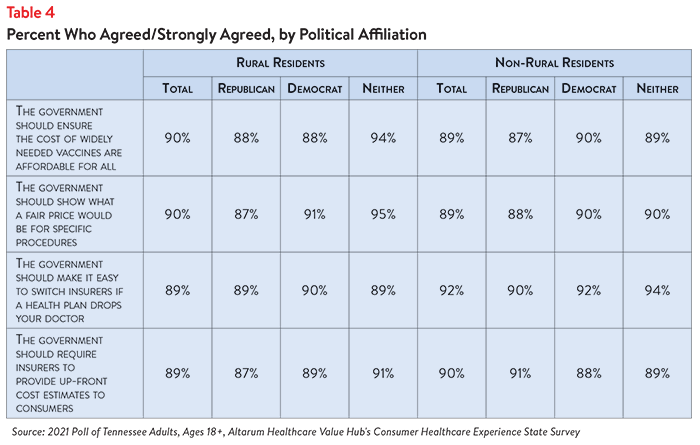
Large shares of both rural and non-rural Tennessee residents reported high levels of worry about affording healthcare in the future. However, rural residents experience slightly higher levels of worry—eight in ten rural respondents (80%) reported being “worried” or “very worried” about one of more of the following topics, compared to 76% of non-rural residents:
Dissatisfaction with the Health System and Support for Change
In light of these healthcare affordability concerns, it is not surprising that both non-rural and rural Tennessee residents were extremely dissatisfied with the health system. More than 7 in 10 rural residents (71%) and 6 in 10 non-rural residents (65%) agreed or strongly agreed that “the system needs to change,” compared to 36% of both non-rural and rural residents who agreed or strongly agreed that “we have a great healthcare system in the U.S.”
Tennessee adults do see a role for themselves in addressing healthcare affordability problems. Both non-rural and rural residents reported actions they have already taken, like researching the cost of a drug beforehand (56% of non-rural residents/60% of rural residents), as well as actions they should be taking. Sixty-eight percent of rural adults and 69% of non-rural adults believed that taking better care of their personal health is one of the top things they can do personally to address affordability. In addition, 77% said they would switch from a brand to an equivalent generic drug if given a chance (75% of rural residents/79% of non-rural residents).
But, in far greater numbers, Tennessee adults see government as the key stakeholder that needs to act to address health system problems. Examples of strategies that received support across party lines included:
The high burden of healthcare affordability, along with high levels of support for change, suggest that elected leaders and other stakeholders need to make addressing healthcare costs a top priority. Moreover, the current COVID crisis is leading state residents to take a hard look at how well health and public health systems are working for them, with strong support for a wide variety of actions. Annual surveys can help assess whether or not progress is being made.
Notes
1. We received too few responses at the regional level to provide a reliable estimate for this statistic, however these respondents are represented in the overall “burdened” population.
For survey methodology and state-wide data, see www.healthcarevaluehub.org/tennessee-state-survey