Nevada Residents Worried about High Drug Costs; Support a Range of Government Solutions
According to a survey of more than 1,130 Nevada adults, conducted from June 21, 2022, to July 8, 2022, respondents are concerned about prescription drug costs and express a strong desire for policymakers to enact solutions.
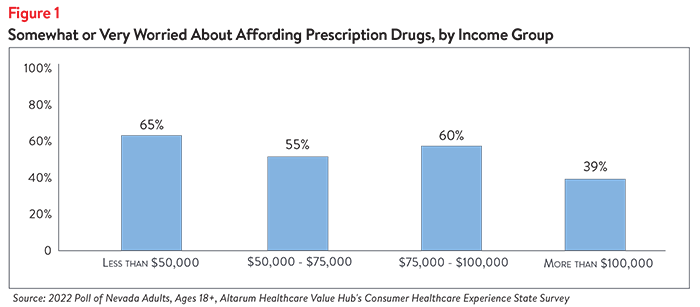
Over half (55%) of survey respondents report being somewhat or very worried about affording the cost of prescription drugs. Worry varied substantially by income group, with respondents in households earning less than $50,000 per year1 reporting the most worry (see Figure 1). However, it is important to note that a large percentage of households earning above $50,000 per year also worry about affording prescription drugs.
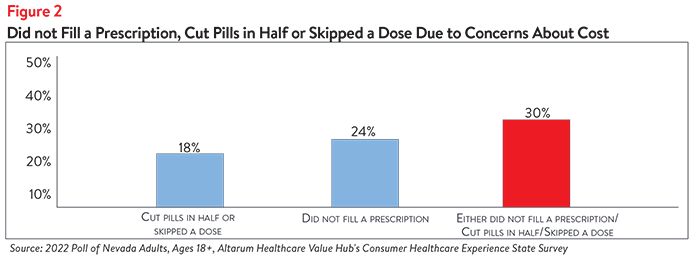
In addition to being worried about prescription drug affordability in the future, many Nevada respondents reported experiencing hardship in the prior 12 months due to the cost of prescription drugs. Nearly 1 in 3 Nevada respondents (30%) did not fill a prescription, cut pills in half or skipped a dose of medicine in the last year due to cost (see Figure 2).
These hardships disproportionately impact people in lower-income households. As Table 1 shows, respondents living in households earning less than $50,000 and those earning between $50,000 and $75,000 per year reported higher rates of rationing their prescription medicines (by not filling a prescription, cutting pills in half or skipping a dose of medicine) than respondents living in higher-income households. These hardships are alarmingly prevalent in middle-income households, as well.
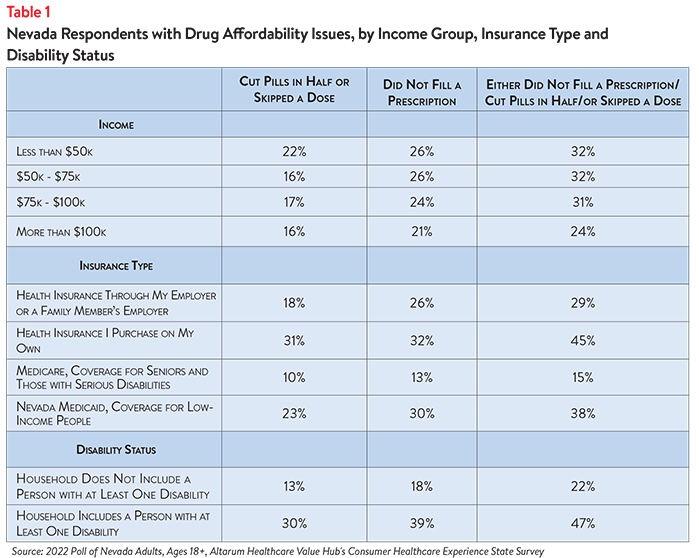
Respondents purchasing health insurance on their own reported the highest rates of rationing medication compared to other insurance types, followed by those with Nevada Medicaid. Finally, respondents living in households with a person with a disability reported notably higher rates of rationing medication due to cost in the past 12 months compared to respondents without a disabled household member.
In light of these prescription drug cost concerns—as well as concerns about high healthcare costs generally2—it is not surprising that Nevada respondents were generally dissatisfied with the health system:
- Just 25% agreed or strongly agreed that “we have a great healthcare system in the U.S.,”
- While 70% agreed or strongly agreed that “the system needs to change.”
When given more than 20 options, the options cited most frequently as being a “major reason” for high healthcare costs were:
- 74%—Hospitals charging too much money
- 73%—Drug companies charging too much money
- 68%—Insurance companies charging too much money
When it comes to tackling high drug costs, Nevada respondents endorsed a number of prescription drug-related strategies:
- 91%—Require drug companies to provide advanced notice of price increases and information to justify those increases
- 91%—Cap out-of-pocket costs for life-saving medications, such as insulin
- 89%—Authorize the Attorney General to take legal action to prevent price gouging or unfair prescription drug price hikes
- 89%—Prohibit drug companies from charging more in the U.S. than abroad
- 86%—Create a Prescription Drug Affordability Board to examine the evidence and establish acceptable costs for drugs
Moreover, there is substantial support for government action on drug costs regardless of the respondents’ political affiliation (see Table 2).
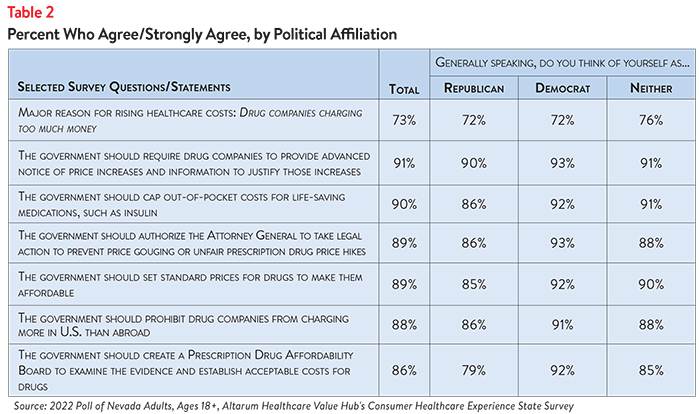
While Nevada respondents are united in calling for the government to address high drug costs, they also see a role for themselves:
- 78% would switch from a brand name to an equivalent generic drug if given a chance
- 55% have tried to find out the cost of a drug beforehand
Conclusion
The high burden of healthcare and prescription drug affordability, along with high levels of support for change, suggest that elected leaders and other stakeholders need to make addressing this consumer burden a top priority. Moreover, the COVID crisis has led state residents to take a hard look at how well health and public health systems are working for them, with strong support for a wide variety of actions. Annual surveys can help assess whether or not progress is being made.
Notes
1. Median household income in Nevada was $62,043 (2016-2020). U.S. Census, Quick Facts. Retrieved from: https://www.census.gov/quickfacts/NV
2. For more detailed information about healthcare affordability burdens facing Nevada respondents, please see: Healthcare Value Hub, Nevada Residents Struggle to Afford High Healthcare Costs; Worry About Affording Healthcare in the Future; Support Government Action Across Party Lines, Data Brief No. 127.
Methodology
Altarum’s Consumer Healthcare Experience State Survey (CHESS) is designed to elicit respondents’ unbiased views on a wide range of health system issues, including confidence using the health system, financial burden and views on fixes that might be needed.
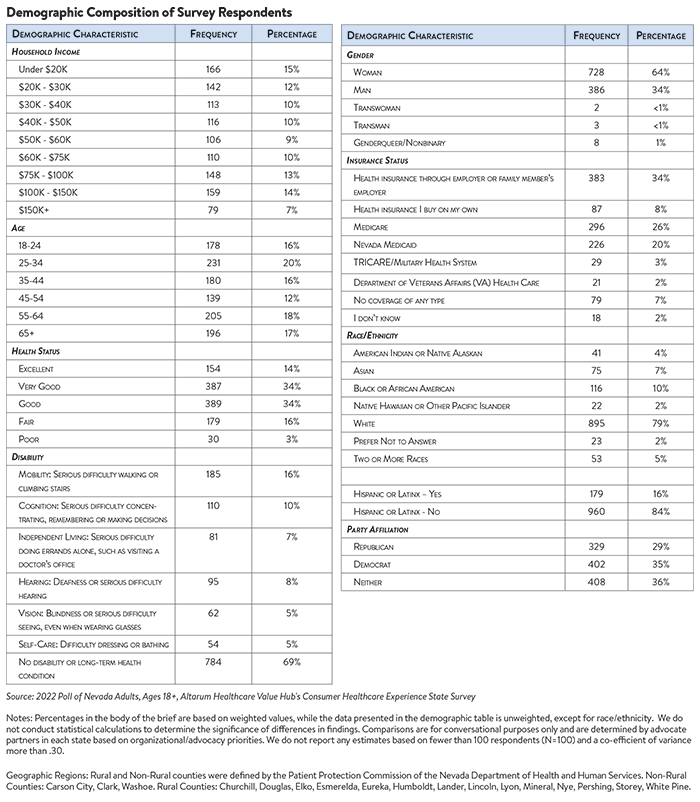
The survey used a web panel from Dynata with a demographically balanced sample of approximately 1,371 respondents who live in Nevada. The survey was conducted in English or Spanish and restricted to adults ages 18 and older. Respondents who finished the survey in less than half the median time were excluded from the final sample, leaving 1,139 cases for analysis. After those exclusions, the demographic composition of respondents was as follows, although not all demographic information has complete response rates: