Michigan Residents Struggle to Afford High Healthcare Costs in Both Rural and Non-Rural Areas
A survey of over 920 Michigan adults, conducted from October 20, 2021 to December 16, 2021, found that people living in non-rural areas of Michigan experience slightly greater healthcare affordability burdens than people living in rural areas of the state. Roughly 6 in 10 (58%) non-rural adults experienced one or more of the following healthcare affordability burdens in the prior 12 months, compared to 5 in 10 (54%) rural adults.
Delaying or Forgoing Healthcare Due to Cost
Nearly half (46%) of rural Michigan adults encountered one or more cost-related barriers to getting healthcare during the prior 12 months, compared to a slightly higher 52% of non-rural Michigan adults. The percentage of people who delayed or skipped needed care varied by service type (see Table 1). Geographic differences in rationing care were highest for mental healthcare and/or addiction treatment and prescription drugs, with non-rural residents more likely than rural residents to report delaying or forgoing these forms of care due to cost.
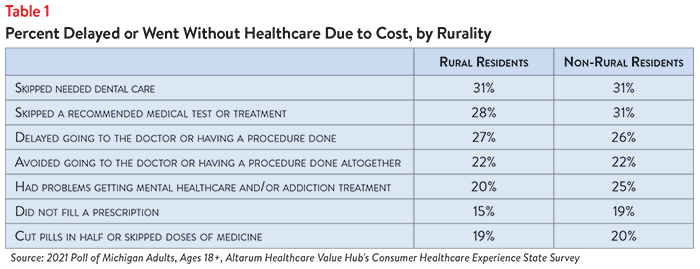
Additionally, non-rural residents more frequently cited cost as a primary reason for not getting medical care (22% of non-rural residents versus 17% of rural residents), while rural residents were more likely to report difficulty getting an appointment as a major barrier to care (20% of rural residents versus 17% of non-rural residents). Cost and difficulty getting an appointment exceeded a host of other barriers like transportation and lack of childcare for both rural and non-rural Michigan adults.
Struggling to Pay Medical Bills
Other times, Michigan adults got the care they needed but struggled to pay the resulting bill. One-third (32%) of rural Michigan adults experienced one or more of the following struggles to pay their medical bills in the prior 12 months, compared to 34% of non-rural Michigan adults (see Table 2).
High Levels of Worry About Affording Healthcare in the Future
Large shares of both rural and non-rural residents reported worrying about affording healthcare in the future. A slightly higher percentage of rural residents (80%) reported being “worried” or “very worried” about one or more of the following topics, while 77% of non-rural residents reported being “worried” or “very worried” (see Table 3).
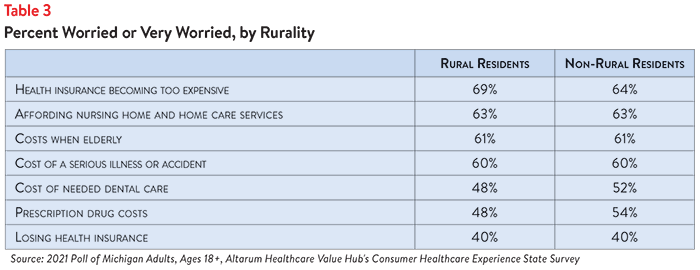
Rural residents were more likely than non-rural residents to worry about healthcare becoming too expensive, while non-rural residents were more likely to worry about the cost of dental care and prescription drugs. Worry about affording nursing home and home care services, the cost of a serious illness or accident, costs when elderly and losing health insurance did not vary by geographic setting.
Dissatisfaction with the Health System and Support for Change
In light of these healthcare affordability concerns, it is not surprising that both rural and non-rural Michigan adults reported being dissatisfied with the health system. Just 32% of rural and 41% of non-rural residents agreed or strongly agreed that “we have a great healthcare system in the U.S.,” while 76% of rural and 75% of non-rural residents agreed or strongly agreed that “the system needs to change.” There are also high levels of support for various government-led policy solutions, regardless of geographic location and political affiliation (see Table 4).
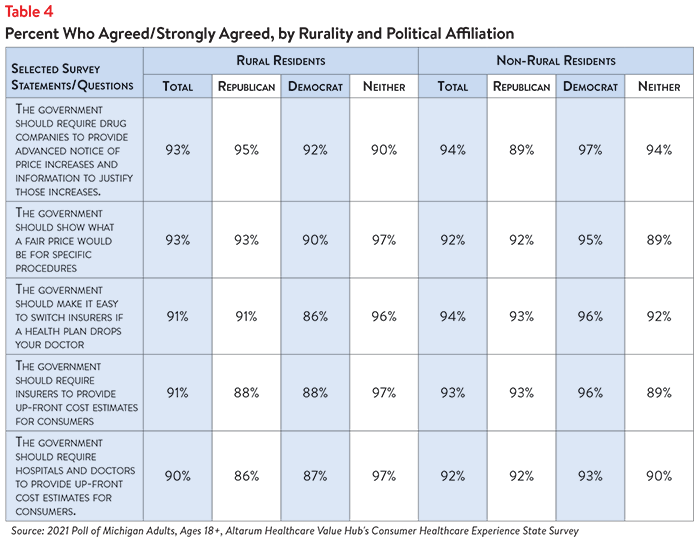

Michigan adults also see a role for themselves in addressing healthcare affordability problems. Both rural and non-rural residents reported actions they have already taken, like researching the cost of a drug beforehand (49% of rural residents and 58% of non-rural residents), as well as actions they should be taking. Sixty-five percent of rural adults and 66% of non-rural adults believe that taking better care of their personal health is one of the top things they can do personally to address affordability. Additionally, many said they would switch from a brand name to an equivalent generic drug if given a chance (78% of rural residents and 72% of non-rural residents).
The high burden of healthcare affordability, along with high levels of support for change, suggest that elected leaders and other stakeholders need to make addressing healthcare costs a top priority. Moreover, the current COVID crisis is leading state residents to take a hard look at how well health and public health systems are working for them, with strong support for a wide variety of actions. Annual surveys, such as this one, can help assess whether or not progress is being made.
Methodology
Altarum’s Consumer Healthcare Experience State Survey (CHESS) is designed to elicit respondents’ unbiased views on a wide range of health system issues, including confidence using the health system, financial burden and views on fixes that might be needed.
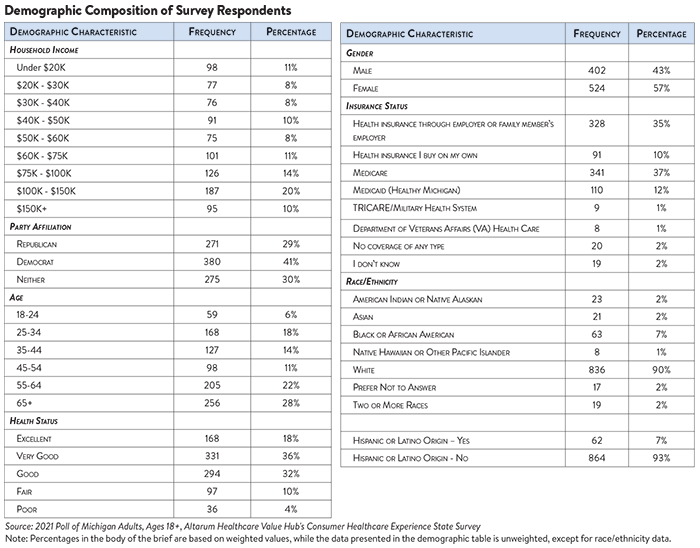
The survey used a web panel from Dynata with a demographically balanced sample of approximately 1,000 respondents who live in Michigan. The survey was conducted in English or Spanish and restricted to adults ages 18 and older. Respondents who finished the survey in less than half the median time were excluded from the final sample, leaving 926 cases for analysis. After those exclusions, the demographic composition of respondents was as follows, although not all demographic information has complete response rates: