Improving Value
Consumer/Patient Incentives
Efforts to address our nation’s health care value problems by changing consumer behaviors often over-estimate consumers’ role in these problems and their ability to drive solutions. Most notably, consumer-facing cost-reduction strategies, like price transparency, are unlikely to significantly lower national health care spending, given the relatively small portion of spending that is directed by consumers.
Nevertheless, evidence suggests that consumers can play a role in improving quality and making health care more patient-centered, with the proper incentives.
Consumers Direct a Small Portion of National Health Care Spending
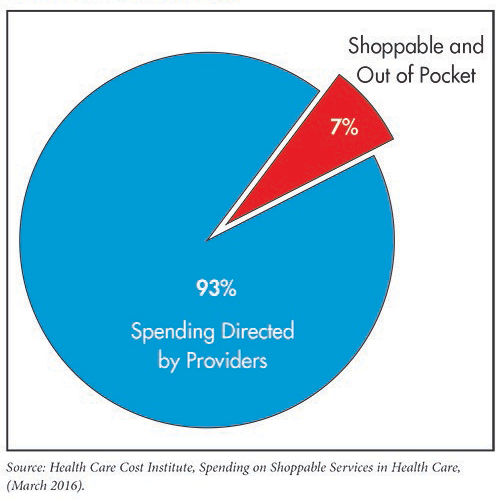
Consumers’ out-of-pocket spending amounts to 15 percent or less of our nation’s health care bill. Out-of-pocket spending on shoppable services (i.e. services for which consumers have the time and information necessary to make an informed decision) accounts for 7 percent or less of the national spend.1 Given the relatively small impact that consumers and patients have on national health care spending, it is unlikely that significant savings would be achieved by increasing consumer-facing price transparency and increasing consumers’ “skin in the game” to incentivize them to shop for lower cost providers.
Furthermore, studies show that, once a consumer initiates care with a provider, the resulting course of treatment seldom varies, regardless of financial incentives. This is presumably because the provider is directing the treatment plan.2
Consumers Direct a Small Percentage of Health Care Spending
Consumer-Facing Strategies Use Financial and Non-Financial Approaches
Strategies that attempt to reduce wasteful health care spending via consumers often use financial incentives, although there is a growing recognition of a role for non-financial incentives, as well.
One of the most common, and most studied, approaches is the use of high deductible health plans (HDHPs). Despite the widespread availability of HDHPs, the evidence is clear that HDHPs do not motivate patients to consume only high-value care. Instead, patients enrolled in these plans reduce their use of both low- and high-value care rather than attempting to comparison shop.
Additionally, research shows that consumers take a very nuanced approach to making health care decisions based on price. They are generally interested in knowing what their out-of-pocket cost will be (for the entire bundle of services that they will eventually receive) for budgeting purposes and to avoid surprises. However, patients don’t necessarily believe that price tag should influence whether or not they should get needed care.3
In contrast, non-financial approaches are somewhat understudied, especially with respect to strategies that aim to steer patient choice (for example, provider quality reports). Studies suggest that public reporting of health care quality information does not significantly affect consumers’ selection of health care providers. This is likely due, in part, to the fact that many people are unaware of the extent to which health care quality varies, thus reducing the motivation to seek such information.4 However, limited evidence suggests that quality information is more effective than price information when it comes to influencing patient decision-making.5
Additionally, patient shared decision-making (PSDM)—a process in which health care providers and patients collaborate to make decisions about the care that patients receive—has been shown to improve patient-doctor communications, improve outcomes and increase patient and physician satisfaction.
Table 1 (below) links to evidence surrounding consumer-facing strategies that aim to inform patient decision-making, enhance patient experience or reduce costs. Given that the evidence is poor for many of these strategies (for example, HDHPs and wellness programs), greater attention must be paid to approaches that are evidence-based. We must also be realistic about the role that patients can play in certain aspects of health system transformation. In some cases, such as lowering national health care spending, their role is limited.
Table 1: Consumer-Facing Strategies to Improve the Health Care System
| Points at which Consumers Engage with the Health Care System | Strategy | Emphasizes Financial Incentives | Emphasizes Non-Financial Incentives |
| Self-Care | Environmental Nudges | X | |
| Wellness Incentives | X | ~ | |
| Public Prevention Programs, including Sin Taxes | X | X | |
| Choosing a Health Plan | Improving Comparative Information About Health Plans | X | X |
| Initiating Treatment | Provider Quality Reports | X | |
| Shared Decision Making & Patient Activation | X | ||
| High Deductible Health Plans | X | ||
| Health Care Price Transparency | X | ||
| Drug Formulary Design | X | ||
| Value-Based Insurance Design | X | ||
| Reference Pricing | X | ||
| Narrow Networks/ Tiered-Provider Networks/Selective Contracting | X | ~ |
Note: See our ingographic on Consumer Health Care Engagement Points.
Notes
1. A "shoppable healthcare service" is typically scheduled in advance, has more than one provider in a market that can perform the service and there is price data available to compare different providers. Ideally, the patient also would have some information on each provider's quality of care, or at lease some reasonable assurance that quality does not vary much. See: Health Care Cost Institute, Spending on Shoppable ervices in Health Care (March 2016). See also: Frost, Amanda, David Newman and Lynn Quincy, "Health Care Consumerism: Can the Tail Wag the Dog?" Health Affairs Blog (March 2, 2016).
2. James, Julia, "Health Policy Brief: Patient Engagement," Health Affairs (February 14, 2013).
3. Bullock, Andrea J., et al., "Understanding Patients' Attitudes Toward Communication About the Cost of Cancer Care," Journal of Oncology Practice, Vol. 8, No. 4 (July 1, 2012).
4. Yegian, Jill Mathews, et al., "Engaged Patients Will Need Comparative Physician-Level Quality Data and Information About Their Out-of-Pocket Costs," Health Affairs, Vol. 32, No. 2 (February 2013).
5. Hibbard, Judith H., et al., "An Experiment Shows That a Well-Designed Report on Costs and Quality Can Help Consumers Choose High-Value Health Care," Health Affairs, Vol. 31, No. 3 (March 2012).