Respondents in the West Virginia and Surrounding Appalachian Counties Region Bear Healthcare Affordability Burdens Unequally; Distrust of/Disrespect by Healthcare Providers Leads Some to Delay/Go Without Needed Care
A survey of more than 1,100 adult respondents from the West Virginia and Surrounding Appalachian Counties (WVSAC) Region,1 conducted from September 26 to November 4, 2022, found that:
- Three in five (64%) of WVSAC respondents have experienced one or more healthcare affordability burdens in the past 12 months. Four in five (84%) worry about affording some aspect of healthcare now or in the future.
- Respondents living in households with a person with a disability more frequently reported affordability burdens than respondents without a disabled household member, including: rationing medication due to cost (39% versus 24%); delaying or going without care due to cost (70% versus 49%); and going into medical debt, depleting savings or sacrificing basic needs due to medical bills (57% versus 32%).
- Forty-five percent of respondents of color skipped needed medical care due to distrust of or feeling disrespected by healthcare providers, compared to 18% of white respondents.
- Fifty-five percent of all respondents think that people are treated unfairly based on their race or ethnic background somewhat or very often in the U.S. healthcare system.
Differences in Affordability Burdens and Concerns
Race
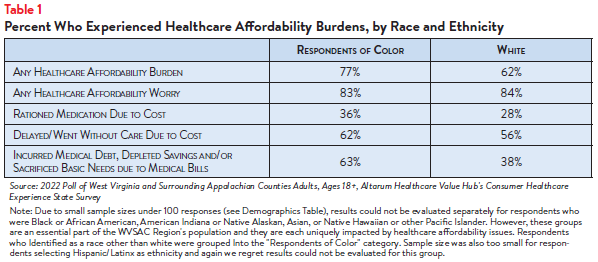
Racial disparities in healthcare are well-documented and affordability issues impact access to care and financial burdens for communities of color, particularly Black and Hispanic/Latinx communities.2,3 In the WVSAC Region, respondents of color reported higher rates of affordability burdens than white respondents, including higher rates of rationing medication due to cost; delaying or going without care due to cost; incurring medical debt, depleting savings or sacrificing basic needs (like food, heat, and housing) due to medical bills (see Table 1).
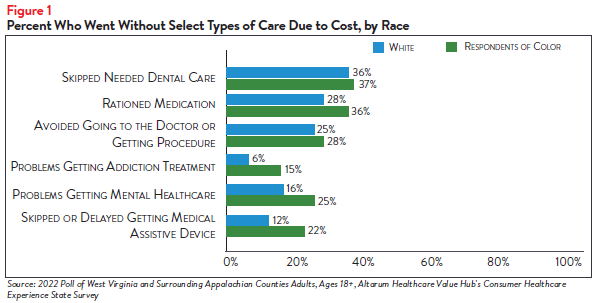
In addition to rationing medication, respondents of color more frequently reported avoiding going to the doctor or getting a procedure and delaying/going without medical assistive devices due to cost, alongside problems getting addiction treatment and going without dental care (see Figure 1).4
Income
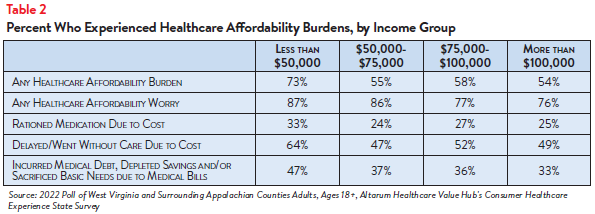
The survey also revealed differences in how WVSAC Region respondents experience healthcare affordability burdens by income. Unsurprisingly, respondents at the lowest end of the income spectrum most frequently reported affordability burdens, with almost three-quarters (73%) of those with household incomes of less than $50,000 per year reporting struggling to afford healthcare in the past 12 months (see Table 2). Still, over half of respondents living in middle- and higher-income households reported struggling to afford some aspect of coverage or care, demonstrating that affordability problems go far up the income ladder. At least 75% of respondents in each income group reported being worried about affording healthcare either now or in the future.
Respondents living in lower-income households also more frequently reported rationing care due to cost. Well over half (64%) of lower-income earners reported delaying or going without at least one healthcare service or treatment due to cost in the past year, compared to roughly half (49%-52%) of those earning over $75,000. Additionally, 1 in 3 (33%) of respondents with household incomes of $50,000 or less reported not filling a prescription, skipping doses of medicines or cutting pills in half due to cost, compared to roughly 1 in 4 respondents in other income brackets.
Lower-income individuals also most frequently reported financial consequences after receiving healthcare services—forty-seven percent either went into medical debt, depleted their savings or sacrificed other basic needs (like food, heat or housing) due to medical bills, compared to 33% of those earning over $100,000.
Disability Status
People with disabilities interact with the healthcare system more often than those without disabilities and, as a result, tend to face more out-of-pocket costs.5 Additionally, people who receive disability benefits face unique coverage challenges that impact their ability to afford needed care, such as the possibility of losing coverage if their household income or assets increase over a certain amount (for example, after getting married).6
WVSAC Region respondents who have a disability or who live with a person with a disability more frequently reported a diverse array of affordability burdens compared to their counterparts (see Table 3). These individuals also more frequently reported worrying about healthcare affordability in general (87% versus 82%) and losing health insurance (42% versus 26%).
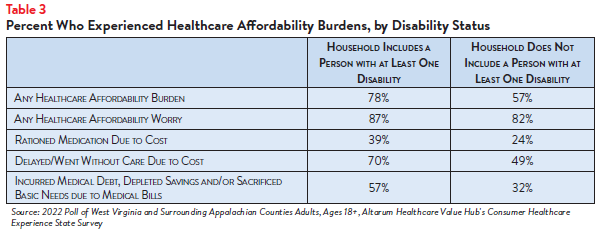
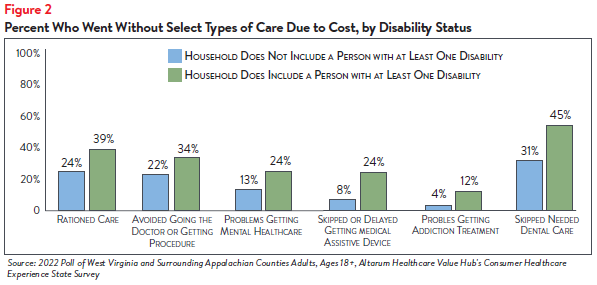
Those with disabilities also face healthcare affordability burdens unique to their disabilities—24% of respondents reporting a disability in their household delayed getting a medical assistive device such as a wheelchair, cane/walker, hearing aid or prosthetic limb due to cost. Just 8% of respondents without a person with a disability (who may have needed such tools temporarily or may not identify as having a disability) reported this experience (see Figure 2). Similarly, 24% of respondents reporting a disability in their household also reported problems getting mental healthcare compared to 13% of households without a person with a disability.
Gender
The survey also surfaced differences in healthcare affordability burdens and worry by gender. Women who responded to the survey more frequently experienced at least one affordability burden in the past year than men (68% versus 61%, respectively) (see Table 4). While women more frequently reported delaying or going without care due to cost in general, both men and women reported rationing their medications by not filling a prescription, skipping doses or cutting pills in half, and incurred medical debt, depleted savings and/or sacrificed basic needs due to medical bills at similar rates.
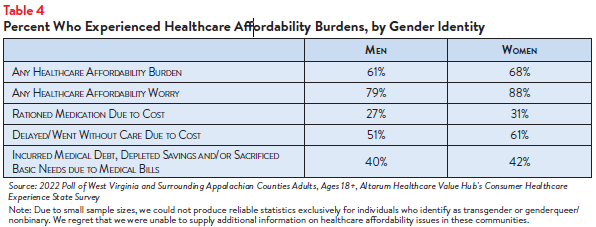
While most respondents of both genders reported being somewhat or very concerned about affording some aspect of coverage or care, a higher percentage of women reported this worry than men (88% versus 79%, respectively).
Due to the small sample size, this survey could not produce reliable estimates exclusively for transgender or genderqueer/nonbinary respondents. However, it is important to note that these groups experience unique healthcare affordability burdens—1% of survey respondents (9 respondents) reported that they or a family member had trouble affording the cost of gender-affirming care, such as hormone therapy or reconstructive surgery.
Distrust and Disrespect in the Health System
Whether a patient trusts and/or feels respected by their healthcare provider may impact whether they seek needed care. In the WVSAC Region, more than 1 in 3 (35%) of respondents reported that their provider never, rarely or only sometimes treats them with respect. When asked why they felt healthcare providers did not treat them with respect, nearly half of respondents cited their income or financial status (49%), followed by a disability or physical, mental or cognitive condition (26%), race (21%), ethnic background or culture (16%), and gender/gender identity (15%). In lesser numbers, respondents cited sexual orientation (12%) and experience with violence or abuse (8%) as reasons for the disrespect.
Respondents of color and those with a person with a disability in their household more frequently reported distrust in and feeling disrespected by their healthcare providers than their white or non-disabled counterparts (see Table 5). These respondents also more frequently reported going without medical care due to that distrust and/or disrespect. Forty-five percent of respondents of color reported skipping needed medical care due to distrust of or feeling disrespected by healthcare providers, compared to 18% of white respondents. Thirty-six percent of respondents who have a disability or are living with a person with a disability reported going without care due to distrust or disrespect, compared to 15% of those without a household member with a disability.
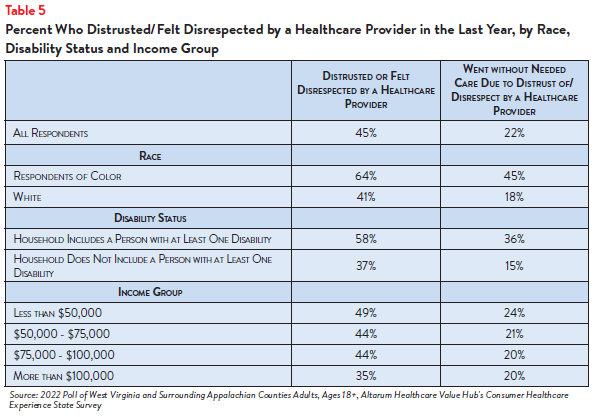
Respondents earning less than $50,000 most frequently reported distrust/disrespect, as well as having gone without care due to distrust/disrespect compared to the other income groups. Interestingly, however, respondents in higher income groups also reported high rates of distrust/disrespect and having gone without care.
Individual and Systemic Racism
Respondents perceived that both individual and systemic racism exist in the U.S. healthcare system. Fifty-five percent of respondents believe that people are treated unfairly based on their race or ethnic background, either somewhat or very often. When asked what they think causes healthcare systems to treat people unfairly based on their race or ethnic background:
- 19% cited policies and practices built into the healthcare system;
- 22% cited the actions and beliefs of individual healthcare providers; and
- 44% believe it is an equal mixture of both
Dissatisfaction with the Health System and Support for Change
Given this information, it is not surprising that 68% of respondents agree or strongly agree that the U.S. healthcare system needs to change. Understanding how the healthcare system disproportionately harms some groups of people over others is key to creating a fairer and higher value system for all.
Making healthcare affordable for all residents is an area ripe for policymaker intervention, with widespread support for government-led solutions across party lines. For more information on the types of strategies state residents want their policymakers to pursue, see: West Virginia Residents Struggle to Afford High Healthcare Costs; Worry About Affording Healthcare in the Future; Support a Range of Government Solutions Across Party Lines, Healthcare Value Hub, Data Brief No. 143 (January 2023).
Notes
- The surrounding Appalachian counties in this region are in Maryland, Pennsylvania, Ohio, Virginia and Kentucky.
- Fadeyi-Jones, Tomi, et al., High Prescription Drug Prices Perpetuate Systemic Racism. We Can Change It, Patients for Affordable Drugs Now (December 2020), https://patientsforaffordabledrugsnow.org/2020/12/14/drug-pricing-systemic-racism/
- Kaplan, Alan and O’Neill, Daniel, “Hospital Price Discrimination Is Deepening Racial Health Inequity,” New England Journal of Medicine—Catalyst (December 2020), https://catalyst.nejm.org/doi/full/10.1056/CAT.20.0593
- A small share of respondents also reported barriers to care that were unique to their ethnic or cultural backgrounds. Two percent reported not getting needed medical care because they couldn’t find a doctor of the same race, ethnicity or cultural background as them or they couldn’t find a doctor who spoke their language.
- Miles, Angel L., Challenges and Opportunities in Quality Affordable Health Care Coverage for People with Disabilities, Protect Our Care Illinois (February 2021), https://protectourcareil.org/index.php/2021/02/26/challenges-and-opportunities-in-quality-affordable-health-care-coverage-for-people-with-disabilities/
- A 2019 Commonwealth Fund report noted that people with disabilities risk losing their benefits if they make more than $1,000 per month. According to the Center for American Progress, in most states, people who receive Supplemental Security are automatically eligible for Medicaid. Therefore, if they lose their disability benefits they may also lose their Medicaid coverage. Forbes has also reported on marriage penalties for people with disabilities, including fears about losing health insurance. Seervai, Shanoor, Shah, Arnav, and Shah, Tanya, The Challenges of Living with a Disability in America, and How Serious Illness Can Add to Them, Commonwealth Fund, New York City, NY. (April 2019), https://www.commonwealthfund.org/publications/fund-reports/2019/apr/challenges-living-disability-america-and-how-serious-illness-can
See also: Fremstaf, Shawn and Valles, Rebecca, The Facts on Social Security Disability Insurance and Supplemental Security Income for Workers with Disabilities, Center for American Progress, Washington D.C. (May 2013), https://www.americanprogress.org/article/the-facts-on-social-security-disability-insurance-and-supplemental-security-income-for-workers-with-disabilities/
See also: Pulrang, Andrew, “A Simple Fix For One Of Disabled People’s Most Persistent, Pointless Injustices,” Forbes (April 2020), https://www.forbes.com/sites/andrewpulrang/2020/08/31/a-simple-fix-for-one-of-disabled-peoples-most-persistent-pointless-injustices/?sh=6e159b946b71
Methodology
Altarum’s Consumer Healthcare Experience State Survey (CHESS) is designed to elicit respondents’ unbiased views on a wide range of health system issues, including confidence using the health system, financial burden and possible policy solutions.
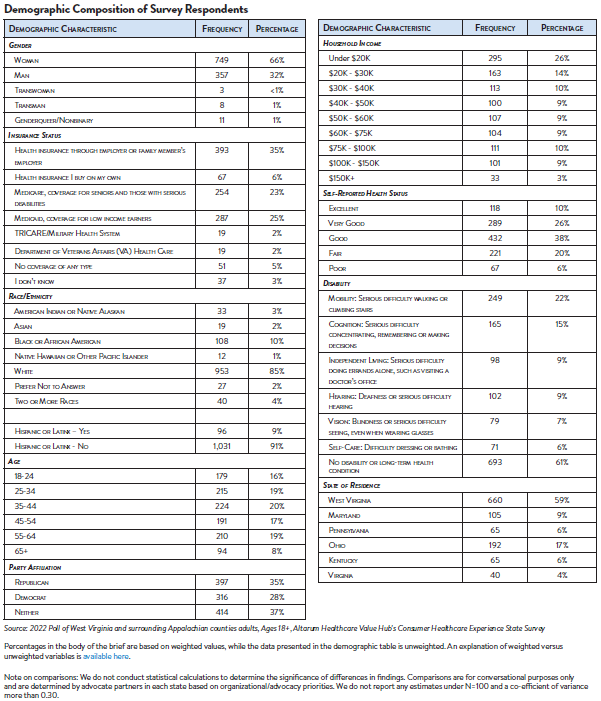
This survey, conducted from September 26 to November 4, 2022, used a web panel from online survey company Dynata with a demographically balanced sample of approximately 1,227 respondents who live in West Virginia and surrounding Appalachian counties. The survey was conducted in English or Spanish and restricted to adults ages 18 and older. Respondents who finished the survey in less than half the median time were excluded from the final sample, leaving 1,127 cases for analysis. After those exclusions, the demographic composition of respondents was as follows, although not all demographic information has complete response rates: